Aim: The aim of this publication is to highlight the diagnostic pitfalls in differentiating retinitis pigmentosa sine pigmento (RPSP) from normal-tension glaucoma (NTG).
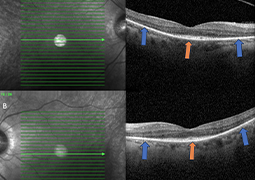
Case Report: A 71-year-old patient was treated for 10 years with topical dual antiglaucoma therapy for NTG, which had been diagnosed based on optic disc pallor, a cup-to-disc ratio of 0.6, normal intraocular pressure, and visual field defects. During the course of subsequent monitoring, the patient developed progressive nyctalopia, concentric visual field constriction, and a marked decline in visual acuity from 1.0 to 0.1. Multimodal imaging, including fundus autofluorescence (FAF), optical coherence tomography (OCT), and perimetry, demonstrated photoreceptor degeneration that did not correlate with glaucomatous optic neuropathy. Genetic testing identified two heterozygous variants in the USH2A gene: one known pathogenic variant (c.11864G>A) and one novel variant (c.12544A>G). Based on these findings and the absence of typical bone spicule pigmentation on fundus examination, a diagnosis of RPSP was determined.
Conclusion: This case underscores the risk of misdiagnosing RPSP as NTG due to overlapping clinical features, and emphasizes the necessity of comprehensive multimodal evaluation, including FAF, OCT, electroretinography, perimetry, and genetic testing, in order to ensure accurate diagnosis and appropriate management.